Lorton, VA(703) 483-8941
Lorton, VA(703) 483-8941
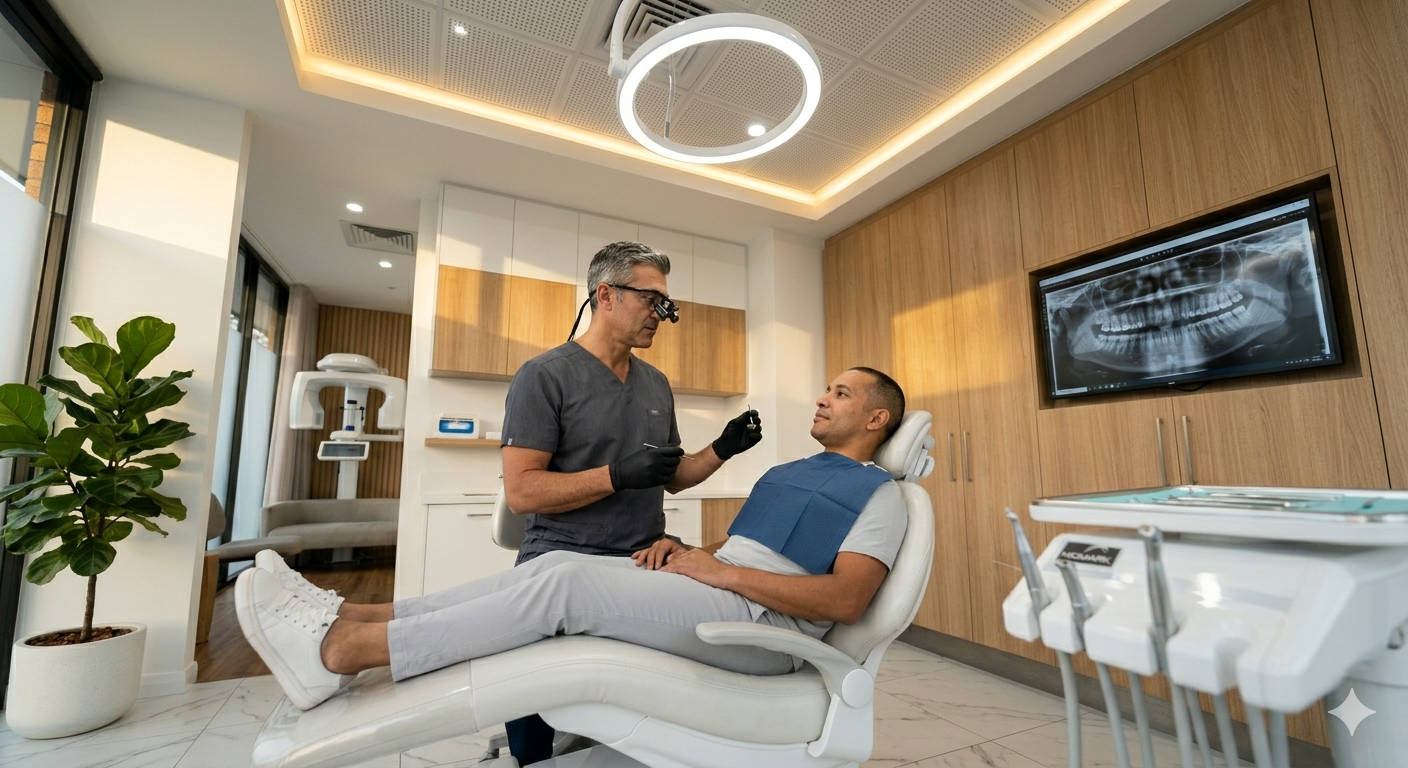
If someone in Lorton, VA, needs oral surgery or a thorough evaluation, this consultation explains what to expect and how it leads to a clear treatment plan tailored to their needs. You’ll learn whether surgery is necessary, what options exist, and how the team will keep comfort and safety top priorities.
The article walks through the initial visit, common concerns addressed at consultation, how to prepare, and modern evaluation tools that make diagnoses more precise. It also covers anesthesia choices, personalized planning, and practical details like insurance and next steps, so whoever is considering care feels informed and confident about moving forward.
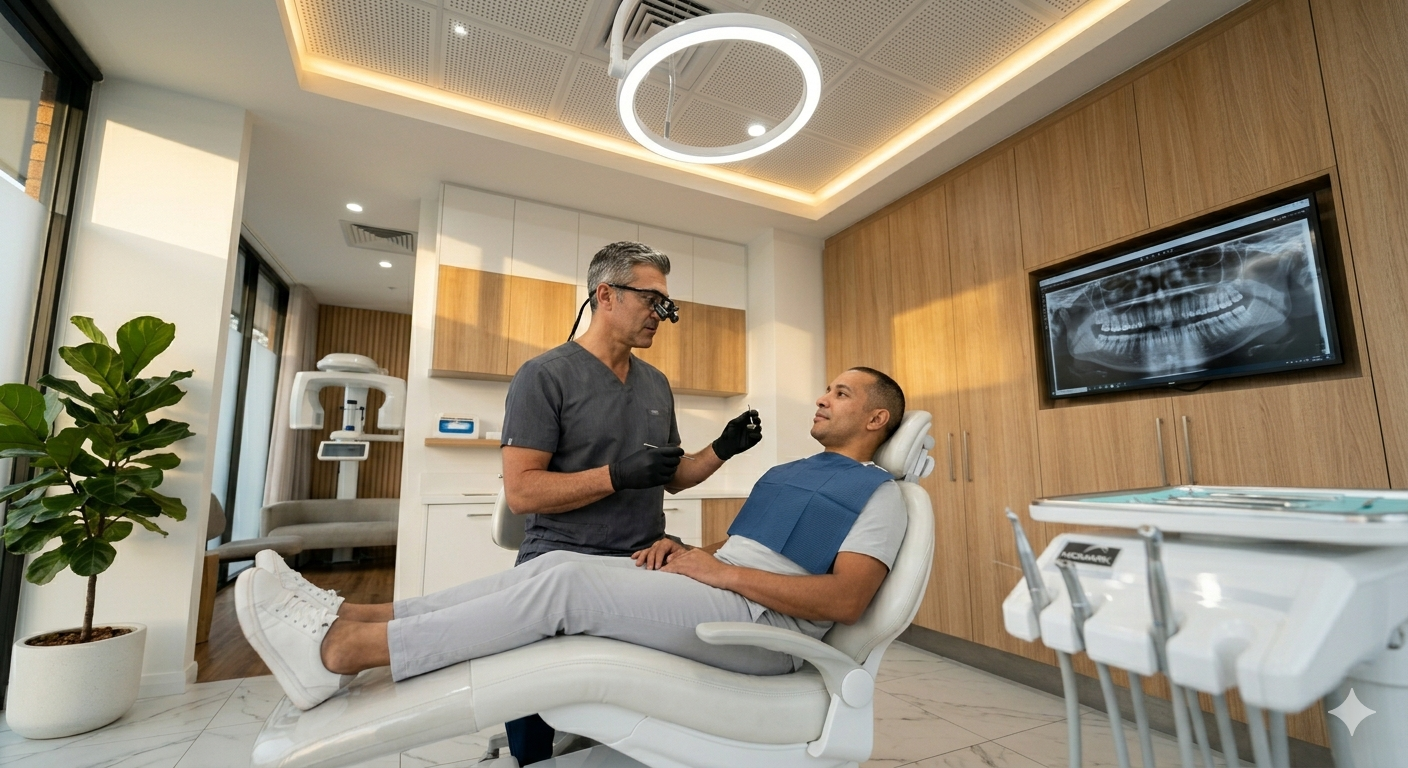
The first visit focuses on clear communication, a thorough exam, and a practical plan tailored to the patient’s needs. Staff will gather information, perform targeted imaging and examination, and discuss treatment options, costs, and comfort measures.
Patients arrive to a calm reception area with seating, reading material, and accessible restrooms. A front-desk team confirms appointment details and insurance, then provides digital or paper forms for consent, contact information, and current medications.
Staff explain privacy practices and estimated visit length. If patients prefer, forms can be completed online before arrival to shorten wait time. The facility usually offers Wi‑Fi and supports mobility needs, such as wheelchair access and ground-floor operatories.
Financial coordinators review insurance benefits and out‑of‑pocket estimates before clinical steps begin. Payment options, financing plans, and preauthorization requirements are explained plainly. This reduces surprises and helps patients plan for next steps.
A clinical assistant escorts the patient to a treatment room and reviews the forms to confirm medications, allergies, and any anxiety concerns. A nurse or dental assistant takes vital signs — blood pressure, pulse, and sometimes oxygen saturation — to ensure safety during procedures.
The oral surgeon conducts a focused exam of the mouth, jaw, and bite, often using intraoral photos and 3D or panoramic x‑rays. Findings are explained in everyday language, pointing out the issue, cause, and urgency. Visuals help patients understand why a procedure might be recommended.
The surgeon discusses anesthesia options — local, nitrous oxide, oral sedation, or IV sedation — and tailors the plan to the patient’s health status and comfort level. They also outline expected recovery time and immediate post‑op instructions so patients know what to expect the day of treatment.
The visit includes a detailed review of medical history, current medications, and prior surgeries. Patients should disclose blood thinners, heart conditions, diabetes, pregnancy, and any allergic reactions to medications or latex to avoid complications.
Dental history covers prior extractions, root canals, orthodontics, and any history of dry socket or healing problems. Smoking and vaping habits are discussed because they affect healing and infection risk. The surgeon records all this information in the chart and flags items for coordination with the patient’s physician if needed.
Before concluding, the team confirms any necessary pre‑op tests or medication adjustments, such as antibiotic prophylaxis or temporary cessation of certain drugs. Clear, written preoperative instructions and a phone number for questions are provided to support a smooth, safe procedure.
Patients can expect evaluation and clear treatment options for painful or non-restorable teeth, missing-tooth replacement, and structural or developmental issues that affect chewing, speech, or appearance. The consult typically includes imaging review, medical history, and a tailored care plan that balances function, comfort, and recovery time.
The consultation reviews tooth-by-tooth risks and benefits, using panoramic X-rays or CBCT when needed to map root positions and nerve proximity. For wisdom teeth, the clinician assesses impaction type (soft tissue, partial, full) and signs of infection, pericoronitis, or cyst formation to determine urgency.
They explain anesthesia choices—local, nitrous oxide, or IV sedation—based on medical history and anxiety level. The plan covers expected recovery: swelling timeline, pain control (NSAIDs ± short opioid if necessary), diet progression, and signs that require immediate contact, such as persistent bleeding or numbness.
When a tooth is restorable versus needing extraction, the consult compares outcomes: root canal and crown versus extraction followed by implant or bridge. Costs, timeline for replacement, and preservation of adjacent teeth and bone inform the recommendation.
The consult evaluates bone volume, sinus position, and neighboring tooth health with imaging to determine implant feasibility. They discuss single implants, implant-supported bridges, and full-arch solutions, including staged versus immediate placement and provisional restorations during healing.
Practical details include grafting needs (autograft, allograft, or synthetic bone), sinus lift indications, and expected osseointegration timeline (typically 3–6 months). The team outlines anesthetic approach, follow-up visits, and temporary prosthesis options to maintain aesthetics and function.
Cost breakdowns, warranty or maintenance plans, and oral hygiene requirements for long-term success appear in writing. The clinician also addresses common patient concerns: implant longevity, sensation changes, and alternatives like fixed bridges or removable dentures.
Consultations cover corrective surgeries such as apicoectomy for persistent root infections, alveoloplasty to reshape bone for dentures, and frenectomy for speech or prosthetic problems. Each procedure is explained in terms of purpose, technique, and recovery expectations.
Orthognathic-related referrals or minor jaw procedures are discussed when bite misalignment causes pain, chewing difficulty, or TMJ symptoms. The consult clarifies when collaboration with orthodontists, prosthodontists, or ENT specialists is recommended.
Patients receive a written treatment timeline, risk-benefit discussion, and post-op care instructions emphasizing pain control, oral hygiene adaptations, and follow-up imaging when needed. The clinician encourages questions and schedules next steps to match the patient’s medical needs and lifestyle.
Patients can make the most of their oral surgery consultation by bringing relevant medical information and a prepared list of questions. Clear communication about medications, symptoms, and expectations helps the surgeon create a safe, personalized plan.
Suggests asking about the specific diagnosis and why a particular procedure is recommended. They should ask: “What is the exact name of the procedure?” and “What are the risks and common complications?”
Patients should request details on anesthesia: “Will I have local, IV sedation, or general anesthesia?” and “Who will monitor my vitals during the procedure?” These questions clarify safety and recovery expectations.
Cost and logistics matter: “What is the total estimated cost, and what does insurance cover?” and “How long will the appointment and recovery take?” Asking about alternative treatments and second-opinion policies helps patients make informed choices.
Also encourage questions about post-op care: “What pain control and antibiotic plan do you recommend?” and “When can I return to work, drive, or normal eating?” These specifics reduce uncertainty and improve recovery planning.
Bring a current list of medications and supplements, including dosages and timing. Patients should include recent changes, blood thinners, and allergy information to avoid complications.
Carry identification, insurance cards, and any referral or prior imaging (X-rays, CBCT scans) on a USB or printed copies. Having previous dental records speeds diagnosis and prevents duplicate imaging.
Prepare a written medical history and contact information for the primary care physician and any specialists. If the patient uses CPAP, inhalers, or blood pressure monitors, bring device details and usage notes.
Bring a list of personal questions and a notepad to record instructions. If sedation is planned, arrange a responsible adult to drive home and bring a phone number for that person.
The practice uses precise digital tools and 3D imaging to plan procedures, reduce surprises, and improve comfort. These technologies create exact models and clear diagnostic images so the clinician can recommend the least invasive, safest path forward.
Digital intraoral scanners capture a full-color, high-resolution 3D model of the teeth and soft tissues without messy putty. Scans complete in minutes and directly export to planning software, milling centers, or the lab, ensuring crowns, bridges, and surgical guides fit more predictably.
Patients experience less gagging and fewer retakes compared with traditional impressions. The clinician can immediately review occlusion, measure distances, and simulate restorative outcomes on-screen. Files also integrate with CBCT data for coordinated surgical and prosthetic planning.
Clinics using digital impressions often send the scan electronically to specialists or the dental lab, shortening turnaround times. The result: fewer appointments, fewer adjustments, and clearer preoperative communication about expected results.
Cone-beam CT (CBCT) provides volumetric images of bone, nerve canals, and sinus anatomy that panoramic X-rays cannot show. The clinician evaluates bone height, width, and density for implant placement, identifies impacted teeth or root fractures, and maps critical structures to minimize nerve or sinus injury.
Software allows cross-sectional slices, virtual implant placement, and nerve-tracing tools that quantify safe distances in millimeters. This precision supports guided surgery and custom surgical guides that translate the virtual plan into the operatory.
Radiation doses are kept low through focused fields of view and modern protocols. The team reviews images with patients, pointing out findings and explaining how the 3D data changes the treatment plan or staging to enhance safety and outcomes.
Patients should expect clear explanations of sedation levels, monitoring, and pain-control plans before any procedure. The team customizes anesthesia and medications based on medical history, the complexity of the surgery, and the patient’s anxiety level.
Oral surgeons commonly offer three main sedation options: local anesthesia, oral sedation, and IV sedation. Local anesthesia numbs only the surgical area using agents like lidocaine; patients remain awake, can follow instructions, and experience little to no pain.
Oral sedation involves a prescribed pill (usually a benzodiazepine such as diazepam or triazolam) taken before the appointment to reduce anxiety and induce drowsiness; patients may have limited memory of the procedure.
IV sedation provides a deeper, adjustable level of sedation delivered through a vein; it ranges from conscious sedation (patient breathes independently) to deep sedation, and it is monitored continuously by trained staff.
For children or patients with special needs, nitrous oxide (“laughing gas”) or general anesthesia may be recommended. Providers review current medications, allergies, and medical conditions to select the safest option and explain fasting and escort requirements when applicable.
Pain control typically combines intraoperative anesthetics, short courses of oral analgesics, and home-care strategies. Immediately after surgery, surgeons often prescribe or recommend acetaminophen and an NSAID (ibuprofen or naproxen) used together for superior pain relief unless contraindicated.
Stronger opioids are reserved for severe pain and given in limited quantities with clear instructions on duration and safe storage. Ice packs, head elevation, and a soft-food diet reduce swelling and discomfort during the first 48–72 hours.
Patients receive written post-op instructions covering wound care, signs of infection, activity restrictions, and when to call the office. Follow-up visits and available phone support ensure pain stays controlled and recovery progresses as expected.
This practice builds a treatment plan around the patient’s medical history, dental records, and personal goals. The plan balances safety, function, and appearance while explaining timelines, costs, and follow-up care.
The oral surgeon reviews the patient’s chart, recent x-rays, and any periodontal notes from the general dentist before the first surgical visit. They confirm diagnoses such as impacted wisdom teeth, failing implants, or pathology, and discuss previous treatments that might affect surgery (e.g., bisphosphonate use, radiation, or anticoagulant therapy).
They exchange specific imaging and treatment options, often using CBCT scans and annotated images to align surgical access with restorative needs. This coordinated approach sets precise goals — for example, preserving bone for a future implant or planning flap design to protect adjacent crowns.
The team agrees on timing: whether extraction, grafting, and implant placement occur in staged visits or a single operative session. They document responsibilities, postoperative instructions, and who will manage acute complications, so the patient experiences seamless care.
The clinician assesses anatomy, medical conditions, and lifestyle factors to select an individualized technique. For a smoker with thin buccal bone, they might recommend staged socket preservation and delayed implant placement to improve predictability.
They present clear options with pros, cons, and expected recovery time. For instance:
The surgeon addresses patient concerns like anxiety or pain control by offering sedation options and a written pain-management plan. They also provide a step-by-step schedule, itemized cost estimates, and preoperative instructions so the patient knows exactly what to expect and who to contact at each stage.
This section explains common payment choices, what costs most procedures typically involve, and practical steps to reduce out‑of‑pocket expenses. It covers how clinics handle insurance claims, available financing, and ways to use dental benefits effectively.
The practice accepts major dental insurance plans and files claims directly to most carriers to simplify billing for patients. Patients should bring their insurance card and a list of providers’ contact info to the first visit so staff can verify coverage and estimate patient responsibility before treatment.
For uninsured or out‑of‑pocket cases, the office offers itemized estimates and accepts cash, debit, credit cards, and electronic payments. They also provide third‑party financing through partners such as CareCredit or in‑office payment plans with clear terms and monthly payment schedules.
Patients receive written estimates showing procedure codes, provider fees, expected insurance payments, and remaining balance. This transparency helps patients compare options and schedule treatment in phases to manage costs.
Patients should confirm whether procedures are categorized as preventive, basic, or major by their insurer, because coverage percentages and annual maximums differ. For example, routine extractions may fall under “basic,” while oral surgery for impacted teeth could be “major” — checking these categories avoids surprise bills.
Schedule pre‑authorization for major procedures when possible; insurers often require it and it clarifies which portions they will pay. The office staff can submit pre‑authorizations and provide supporting X‑rays and operative notes to speed approvals.
Patients approaching their annual maximum may benefit from timing elective work before year‑end or splitting care between calendar years. Keep a record of used benefits, and request a benefits breakdown from the insurer if coverage details are unclear.
Choosing a nearby oral surgeon gives patients faster access to care, clearer communication, and treatment plans tailored to local needs. Proximity often means clinicians know regional referral networks, insurance particulars, and community health resources that affect treatment timing and cost.
A local specialist treats patients from the same neighborhoods, which shapes practical care decisions. They schedule appointments with an eye toward commuting patterns in Lorton, offer evening or weekend slots for working parents, and coordinate with local primary care physicians and pediatric dentists for shared medical histories.
Clinics often maintain relationships with nearby pharmacies and imaging centers, so prescriptions and CT or panoramic X-rays get processed quickly. Staff typically speak common local languages and understand cultural preferences around consent and pain management, improving patient comfort and compliance.
Patient education focuses on realistic day‑to‑day recovery steps: clear instructions for eating, driving, managing swelling, and returning to work. That hands‑on, geographically aware approach reduces missed appointments and speeds recovery.
Local specialists provide follow-up care that fits patients’ lives, not distant clinic schedules. They set checkups timed to typical recovery milestones—24–72 hour phone checks, one‑week wound exams, and two‑week suture returns—so complications are caught early.
Emergency access matters: nearby offices can offer same‑day or next‑day appointments for post‑op bleeding, infection, or severe pain. Clinics often publish direct phone lines and patient portals for secure messaging and photo uploads, enabling remote assessment and quicker triage.
Continuity extends to preventive plans and referrals. The surgeon coordinates with local dentists for implant restoration or orthodontists for referral-based needs, ensuring treatments progress smoothly without repetitive paperwork or lost imaging.
After the consultation, the team outlines a clear, personalized treatment plan. They explain each procedure, estimated timeline, and cost so patients know what to expect.
Patients receive practical pre- and post-operative instructions to improve comfort and healing. Simple tips cover eating, medications, and activity levels to reduce complications.
A typical plan may include one or more of the following:
Insurance and financing options get reviewed in plain language. Staff helps verify benefits and offers payment plans when necessary.
Follow-up care focuses on prevention and long-term oral health. Routine check-ups, hygiene guidance, and targeted treatments lower the chance of future problems.
They encourage questions at every step and invite patients to call or book a follow-up. Scheduling a consultation makes the next steps simple and supported.
This section answers practical concerns about what happens during a visit, insurance, sedation, implants, referrals, and recovery. It gives clear steps patients can expect and how to prepare for treatment in Lorton, VA.
The surgeon reviews medical and dental history, current medications, and any X-rays or CBCT scans already taken. They perform an exam of the mouth, discuss symptoms or goals, and explain recommended treatment options.
The team will outline a treatment plan with timing, necessary tests, and estimated costs. Patients should bring a list of medications, insurance cards, and any previous dental records or imaging.
Many oral surgery offices accept self-referrals, so patients can call or book online without a dentist’s note. A referral can speed communication between providers but is not always required.
If insurance requires a referral for coverage, the office will notify the patient and help coordinate with the referring dentist. Patients should check their plan’s rules before scheduling.
Candidates are adults with adequate bone to support an implant or enough time and willingness for bone grafting if needed. Good candidates maintain reasonable oral hygiene and control chronic conditions like diabetes.
The surgeon evaluates bone volume with CBCT imaging and checks gum health, smoking habits, and medications that affect healing. They discuss alternative options when implants are not advisable.
Typical options include local anesthesia, oral sedatives (like a prescribed pill), nitrous oxide (laughing gas), and intravenous (IV) sedation. The practice screens medical history and follows ASA guidelines to choose a safe level of sedation.
A trained anesthetic team or the surgeon monitors vitals throughout the procedure. Patients receive clear pre- and post-sedation instructions and must arrange transportation home for moderate to deep sedation.
Costs vary by procedure complexity, materials (for example, implant brand), and need for bone grafting or extractions. The office provides a written estimate after the consultation and breaks down fees for surgery, anesthesia, and follow-up.
Many dental insurance plans cover a portion of oral surgery; medical insurance may help when procedures relate to medical conditions. The billing team verifies benefits, submits claims, and offers financing or payment plans when needed.
Recovery for simple extractions or minor surgery commonly takes a few days to a week; implant surgery and bone grafting can take several weeks to months for full healing. Initial discomfort, swelling, and limited chewing are normal.
Follow written post-op instructions: take prescribed pain medication and antibiotics as directed, use ice packs, stick to soft foods, and avoid smoking. Attend scheduled follow-ups so the surgeon can monitor healing and remove sutures if necessary.